Tailoring Messages for Cross-Cultural Communication: Recommendations for COVID-19 Case Investigators and Contact Tracers
May 11, 2022
Introduction
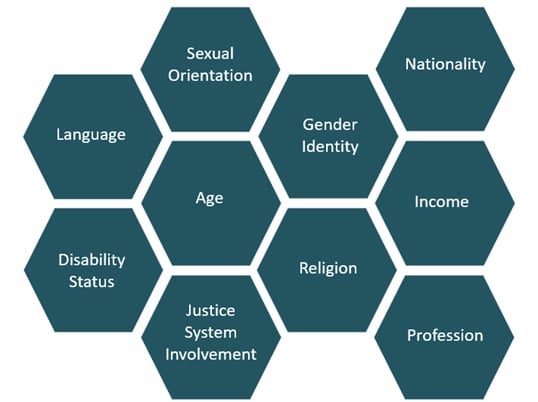 Case investigators and contact tracers must understand and adapt to the culture of people with COVID-19 and their close contacts to conduct effective interviews and follow-up. Culture refers to the learned and shared behavior of a community of people who interact with one another. A person’s culture may be influenced by a several factors, including those listed in the image below.
Case investigators and contact tracers must understand and adapt to the culture of people with COVID-19 and their close contacts to conduct effective interviews and follow-up. Culture refers to the learned and shared behavior of a community of people who interact with one another. A person’s culture may be influenced by a several factors, including those listed in the image below.
Culture helps shape a person’s values, relationships, and understanding of the world around them. For example, some cultures may have different attitudes or beliefs about COVID-19 transmission, vaccination, or treatment. Culture may affect a person’s willingness to identify close contacts or provide a description of those contacts. It may also affect how a person understands and communicates their symptoms, or influence their beliefs about authority figures, health care professionals, and public health. Some residents may mistrust government and public health systems because of injustices they have faced and continue to experience. It’s important that case investigators and contact tracers acknowledge existing fears and concerns, and work with residents to build trust.
This brief overviews the four elements of cross-cultural communication, as well as key principles for inclusive communication. Case investigators and contact tracers should check with their agency for additional resources or support systems to promote culturally inclusive communication.
Four Elements of Cross-Cultural Communication
When interacting with people of different cultures, case investigators and contact tracers should:
- Be aware of your own cultural values: Ask yourself: what are some of your own cultural values? Consider how your prior experiences and beliefs may influence your interactions, and your approach to case investigation and contact tracing. It is important to recognize that you, too, may have pre-existing beliefs about COVID-19 and the cultural groups you work with.
- Be aware of and accept cultural differences: There are similarities and differences between all cultures, but this does not mean that any group is better or worse than one another. It is important to practice cultural sensitivity and treat all people with COVID-19 and their close contacts with respect and compassion. Avoid language that may make the person feel judged or embarrassed.
- Develop cultural knowledge: Be aware of the views and values of the various cultural groups you work with. It may be helpful to ask people with COVID-19 and their close contacts questions such as:
- How do you prefer to be addressed?
- How are important health care decisions made in your family?
- Are there any health care procedures or tests that your culture prohibits?
- Adapt to the cultural context of the person with COVID-19 or their close contact: The person with COVID-19 or their close contact may have different beliefs, values, and preferences. It is important to respect these differences and to adapt your communications accordingly. Understanding what is important to different cultures may help your message resonate.
Let’s Reflect
Think about how you would describe yourself to a stranger. What characteristics or qualities would you mention? They may be a mix of qualities that you are born with (e.g., gender, race) or roles that you play (e.g., occupation, marital status).
How did you decide which characteristics best describe you? How do these characteristics influence what is important to you? What are the advantages or disadvantages of being who you are in your personal life? In your professional life?
Key Principles for Inclusive Communication
When communicating with people with COVID-19 and their close contacts, some key principles to keep in mind include:
- Avoid using adjectives such as “vulnerable,” “marginalized,” and “high-risk.” Instead, use phrases such as “groups that have been marginalized,” or “under-resourced communities.”
- Use person-first language and avoid language that may be dehumanizing.
- Be specific about the group you are referring to. Avoid broad terms such as “minorities.” Behind labels such as “disabled” or “religious minorities” are people with different experiences, beliefs, and values.
- Avoid using terms with violent connotations (e.g., target, tackle, combat, etc.) when referring to people, groups, or communities.
- Avoid unintentionally blaming a group for a behavior. For example, saying “people who refuse vaccination,” could lead to negative assumptions or blame. Instead, consider saying “people who have not yet been vaccinated.”
Resources
- ASTHO and the National Coalition of STD Directors: Making Contact: A Training for COVID-19 Case Investigators and Contact Tracers
- CDC: Cultural and Diversity Considerations
- CDC: Health Equity Guiding Principles for Inclusive Communication
- Virginia Department of Health: COVID-19 Testing and Contact Tracing Health Equity Guidebook