Preventing Fatal Overdoses in Postpartum Populations
May 13, 2020
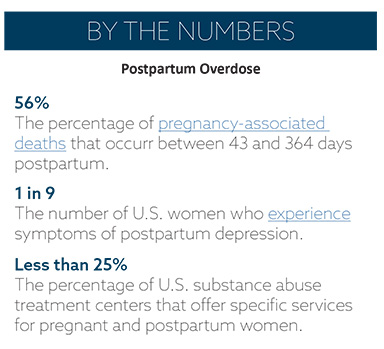
 In 2016, approximately 70% of maternal deaths involving opioids occurred during pregnancy or up to 42 days postpartum. While opioid use during pregnancy has received increased attention in recent years, less attention has been given to overdose- related deaths during the postpartum period. A 2012–2014 study of postpartum women showed declines in overdose-related deaths during pregnancy and a significant increase in overdose-related deaths seven to 12 months postpartum. Women in this study who experienced an overdose were significantly more likely to have had anxiety or depression prior to the overdose than women who didn’t overdose. Access to affordable health care is imperative during the first year following childbirth, when many women struggle with challenges such as sleep deprivation and postpartum depression. However, in the 14 states that have not expanded Medicaid, women lose their coverage just 60 days after giving birth. Additionally, most insurers only provide coverage for one appointment with an obstetrician at six weeks postpartum. These factors result in poorer health outcomes for both mother and child. The American Medical Association, the American College of Obstetricians and Gynecologists, and multiple state maternal mortality review committees have recommended extending Medicaid coverage to 12 months postpartum to improve maternal health outcomes following findings that many maternal deaths, including those linked to overdose and suicide, occur in the postpartum period.
In 2016, approximately 70% of maternal deaths involving opioids occurred during pregnancy or up to 42 days postpartum. While opioid use during pregnancy has received increased attention in recent years, less attention has been given to overdose- related deaths during the postpartum period. A 2012–2014 study of postpartum women showed declines in overdose-related deaths during pregnancy and a significant increase in overdose-related deaths seven to 12 months postpartum. Women in this study who experienced an overdose were significantly more likely to have had anxiety or depression prior to the overdose than women who didn’t overdose. Access to affordable health care is imperative during the first year following childbirth, when many women struggle with challenges such as sleep deprivation and postpartum depression. However, in the 14 states that have not expanded Medicaid, women lose their coverage just 60 days after giving birth. Additionally, most insurers only provide coverage for one appointment with an obstetrician at six weeks postpartum. These factors result in poorer health outcomes for both mother and child. The American Medical Association, the American College of Obstetricians and Gynecologists, and multiple state maternal mortality review committees have recommended extending Medicaid coverage to 12 months postpartum to improve maternal health outcomes following findings that many maternal deaths, including those linked to overdose and suicide, occur in the postpartum period.
Even for those with access to affordable health care, there are still not sufficient services in place to address opioid use disorder in pregnant and postpartum populations. Among the few substance use treatment centers that offer personalized services for these individuals, even fewer provide medication assisted treatment (MAT). Due to this lack of infrastructure, women who suffer from postpartum depression and opioid use disorder are likely to relapse.
Legislative Trends
Recognizing the increase in overdose-related deaths among postpartum women, state legislatures have begun taking action to increase access to services and treatment by expanding Medicaid coverage to include services for postpartum women and extending coverage longer after pregnancy.
In 2019, Colorado’s governor signed a bill authorizing the department of human services to use state funds to provide services to women, including those enrolled in the medical assistance program, who enroll up to one year postpartum in residential substance use disorder treatment services, until such time as those services are covered by the medical assistance program. In addition, the bill extends eligibility for federal approval for substance use disorder treatment services to 12 months postpartum for parenting women. The bill also authorizes the department to request that necessary changes be made to federal waiver programs expanding treatment access for high-risk pregnant and parenting women to further access treatment. Lawmakers justified the policy amendments by acknowledging that a woman’s risk for overdose is highest at seven to 12 months postpartum.
In 2019, several states enacted legislation providing Medicaid coverage for pregnant women to address postpartum depression. In Texas, the governor approved a bill that aimed to improve access to care for Medicaid-enrolled pregnant women with opioid use disorder and their children. Additionally, the bill mandates that enhanced, cost-effective, and limited postpartum care services be provided for all women enrolled in the Healthy Texas Women program, a state Medicaid program.
The District of Columbia enacted legislation requiring Medicaid to provide coverage for pregnant women who meet eligibility requirements for one year postpartum. Missouri, which has not expanded Medicaid, also passed legislation expanding state Medicaid services to women with a history of substance use for up to one year postpartum. West Virginia’s governor signed a bill extending Medicaid coverage to eligible pregnant women and their newborn infants to up to 60 days postpartum.
Illinois enacted a bill extending Medicaid coverage up to one year postpartum—increased from 60 days—and expanding benefits to include coverage for doula services. New Jersey passed legislation naming pregnant women who meet income eligibility requirements as qualified applicants for Medicaid for up to 90 days postpartum. In the current session, other states are considering similar legislation. An Illinois bill would provide coverage for prenatal and postnatal support services during pregnancy and during the 24 month period after pregnancy to women eligible to receive medical assistance. Massachusetts also proposed legislation that would permit doula services before, during, and after childbirth covered by Medicaid. Two Missouri bills (SB788 and HB2574) would allow women who are receiving mental health treatment for postpartum depression to be eligible for MO HealthNet benefits for mental health services for the treatment of postpartum depression for up to 12 additional months.
Looking Ahead
 For states that have expanded Medicaid, future policy trends to reduce overdose and suicide deaths among postpartum women may include implementing MAT and mental health services to provide a more comprehensive care plan for the postpartum population. In states that have not expanded Medicaid, it will be necessary to ensure continuity of care during the postpartum period.
For states that have expanded Medicaid, future policy trends to reduce overdose and suicide deaths among postpartum women may include implementing MAT and mental health services to provide a more comprehensive care plan for the postpartum population. In states that have not expanded Medicaid, it will be necessary to ensure continuity of care during the postpartum period.
Whether or not a state has expanded Medicaid, future state legislation may encourage and enable public health professionals and providers to adopt a holistic approach toward care for postpartum women. According to the American College of Obstetricians and Gynecologists, postpartum care should include appointments with obstetricians three weeks after birth, with a comprehensive appointment to follow up at 12 weeks postpartum. With proper physical and mental health support during the postpartum period, relapse and overdose can be prevented for women with opioid use disorders.